
My nearly 94-year-old mother recently developed a pressure sore on one of her heels. We knew exactly what it was when we saw it, and, thus, were able to catch it in at an early stage before it worsened. Mom also complained about pain in her heel—another clue.
Pressure sores that occur as the result of time in bed are more commonly known as bedsores—and are one of the many physiological perils of too much bed rest. Unfortunately, my mother, who suffers from mild dementia, spends too much time lying in bed, sleeping. She enjoys sleep, and the relief it brings from the tasks of daily living (exercise, showers), and is very difficult to rouse in the morning.
When Mom is in bed, she never changes position. She lies supine (on her back; “prone” is face-down), so that her heels, as well as her elbows, shoulders, tailbone, and other not-very-well-padded areas of her body, bear a lot of pressure.
Bedsores develop when pressure against the skin limits blood flow, thus impairing the delivery of oxygen and other nutrients, such as proteins, vitamins, and minerals, to the affected tissue. Tissue thus deprived becomes damaged and can even die. The skin on Mom’s heel was reddened. Some of it had flaked off, and a small, superficial circular sore had appeared.
My first-aid intervention and pressure-sore prevention for Mom got me thinking about blood and the how-to of the hematological system. (It also got me thinking about the many ghastly consequences of prolonged bed rest or immobility, but that’s grist for another, more intricately detailed column. Deconditioning, impairment, disability: Too much bed rest can devastate the human body.)
When I did the research for my book, Our Parents in Crisis, I learned that the supine position in bed, just by itself, in or out of the hospital, causes 10 percent or more of your body’s total blood volume to be redistributed from the lower extremities to the central circulation. Most of it is diverted to the lungs, but some goes to the head and arms.
Further bloody thoughts led to the following:
COMPONENTS OF BLOOD
The human body contains about five to six liters of blood, or about 1.5 gallons. A liter is a little more than a quart; bodily fluids are not measured in quarts.
You sometimes hear about a person losing a pint—which is half of a quart—of blood. Inasmuch as there are eight pints in a gallon, one pint would represent about 1/12 of the body’s total blood volume.
No doubt you have heard of plasma, which is a key component of blood. Plasma is a clear, yellowish fluid that makes up about 55 percent of your whole blood. Plasma consists of 95 percent water. Its remaining 5 percent contains clotting proteins, antibodies to fight infection, and electrolytes (e.g., sodium, calcium, magnesium, and potassium).
The other 45 percent of your blood’s composition consists of red blood cells (RBCs), also called erythrocytes; white blood cells (WBCs), called leukocytes, of which there are multiple types; and platelets, called thrombocytes.
Plasma fluid carries the erythrocytes, leukocytes, and platelets. It also transports nutrients, hormones, and proteins to the areas of your body that need them and helps to remove waste products from your cells.
Healthy people produce billions of white and red blood cells every hour of every day under normal conditions. In the event of infection, bleeding, or other stressors, new-blood-cell growth increases. The blood-cell production process, called hematopoiesis, occurs mainly in your bone marrow, which is the spongy vascular center inside your bones. The red-blood-cell (RBC) production process is called erythropoiesis.
BLOOD-CELL FUNCTION
Red blood cells contain hemoglobin, the iron-enriched protein that carries oxygen through your arterial (arteries) system to your organs and tissues. Hemoglobin also transports about 10 percent of the carbon dioxide that the red blood cells transport from your organs and tissues back to your lungs through your venous (veins) system.
When the rate of new RBC production equals the rate of old RBC destruction, there is no change in the oxygen-carrying capacity of the blood.
Your capillaries, the body’s smallest blood vessels, connect the arterial and venous blood systems. It is in the capillaries that the exchange of gases (oxygen and carbon dioxide), nutrients, and metabolic waste occurs. Venous blood that carries CO2 and other waste to the lungs is deoxygenated.
Each red blood cell lasts about 120 days. After squeezing repeatedly through small capillaries, RBCs undergo wear-and-tear that cannot be repaired. Your spleen, an organ in the lymphatic system that filters the blood, removes damaged or old RBCs, and your bone marrow produces new cells.
Closely connected with the blood and the circulatory system, the lymphatic system consists of an extensive network of organs, nodes, ducts, and vessels that make and move lymph, a clear fluid containing a high number of lymphocytes, which are a type of leukocyte (white blood cell), from the tissues to the bloodstream. Lymphatic vessels branch throughout your body, in close proximity to blood vessels, and circulate around the interstitial tissues. They drain excess fluid.
White blood cells protect your body from infection and cancer cells and significantly contribute to your inflammatory and allergic responses. They account for about 1 percent of your blood. After being produced in the marrow, they travel through blood and lymphatic vessels to organs such as the spleen, the tonsils, and the lymph nodes. Because some WBCs have life spans of only one to three days, your bone marrow is constantly producing them. The spleen also makes infection-fighting WBCs.
Platelets, which are made in your bone marrow and circulated in your bloodstream, assist in forming clots to stop the bleeding of a damaged blood vessel. They last about eight to 10 days.
HEMOGLOBIN & HEMATOCRIT
You probably are familiar with a routine panel of blood tests known as a complete blood count or CBC. A CBC provides a physician with valuable information about the cells in your blood, especially your RBCs, WBCs, and platelets.
There are two tests within the CBC that I think everyone should know and understand: the first measures the concentration of hemoglobin in your blood and the second assesses the proportion of your red blood cells among all of your blood cells. Both of these tests, which are typically performed on blood samples by an outside laboratory, rather than in your physician’s office, allow an analysis of your blood’s oxygenation.
Oxygenation is critical, as the wound to my mother’s heel demonstrates.
The normal range for hemoglobin is:
13.5 to 17.5 grams per deciliter of blood (135-175 grams per liter), for men
12.0 to 15.5 grams per deciliter of blood (120-155 grams per liter), for women
A hematocrit reading measures the percentage or proportion of red blood cells in your blood, vis-à-vis other blood cells. Having too many or too few RBCs is a sign of certain diseases, such as lymphoma and leukemia, in the event of too few.
Hematocrit values normally range between 42 and 54 percent in men and between 37 and 47 percent in women. With age, average values of hematocrit decrease slightly, but remain within these ranges.
Anemia, a common complaint in older adults, is a deficiency in your blood’s oxygen-carrying capacity, not a single disease. People who are anemic have a low level of hemoglobin in their blood. (For more about hemoglobin testing, see the Mayo Clinic at https://www.mayoclinic.org/tests-procedures/hemoglobin-test/about/pac-20385075.)
The Merck Manual defines anemia as “decreases in red blood cell or hemoglobin resulting from blood loss, impaired production of RBCs, or RBC destruction” and calls it a “sign” of an underlying benign or malignant (cancer) disease or a chronic illness.
So-called iron-deficiency anemia occurs frequently in older people, but it is never normal. Total body and bone marrow stores of iron increase, not decrease, with age.
Anemia may be the tip of an iceberg of dysfunction or illness that an older person with lower physiological reserves can ill afford. Often it signals poor heart or lung function.
(I periodically provide a primer on how the heart works. See my blog on 2/14/18 for my most recent cardiac guide.)
LOW BLOOD-OXYGEN LEVEL
When your arterial blood is low in oxygen, hypoxemia exists. Blood-oxygen saturation can be assessed with a sample of arterial blood. Normal arterial oxygen is about 75 to 100 millimeters of mercury (mm Hg). According to the online Mayo Clinic, any value lower than 60 mm Hg indicates a need for supplemental oxygen.
The oxygen saturation of arterial blood also can be estimated with a pulse oximeter, a small device that you clip to a finger. An oximeter O2 reading under 90 percent is considered low. When I test my mother’s blood O2 with our home pulse oximeter—usually after she’s been short of breath—I’m hoping for a reading between 94 and 100.
Inasmuch as the oximeter reading is indirect and not based on a saturation that would be obtained from arterial blood gas, it should not be considered precise or foolproof.
Blood is just one of the many functional marvels of the human body. It helps to know and to go with its flow.
Be well!
Ann, 2/28/18
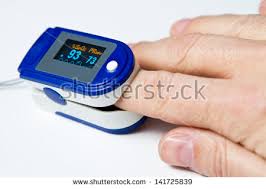
This pulse oximeter shows a 93 percent blood-oxygen saturation level and a 73 hpm pulse.